Authored by:
Shawna Ramey, CPC, CPMA, Post-Acute Medicine Consultant
Health Dimensions Group
In the United States, 84 percent of national health care dollars are spent on people with chronic conditions, and 99 percent of total Medicare costs are incurred by two-thirds of the beneficiaries with two or more chronic illnesses. How many of these patients are you caring for in your practice?
Those statistics should grab your attention. In caring for these complex patients, do you feel you are reimbursed for all of the work completed by you and your clinical staff? If you are like most providers, probably not. The good news is that Medicare has changed the chronic care management (CCM) guidelines and has enhanced your reimbursement opportunities.
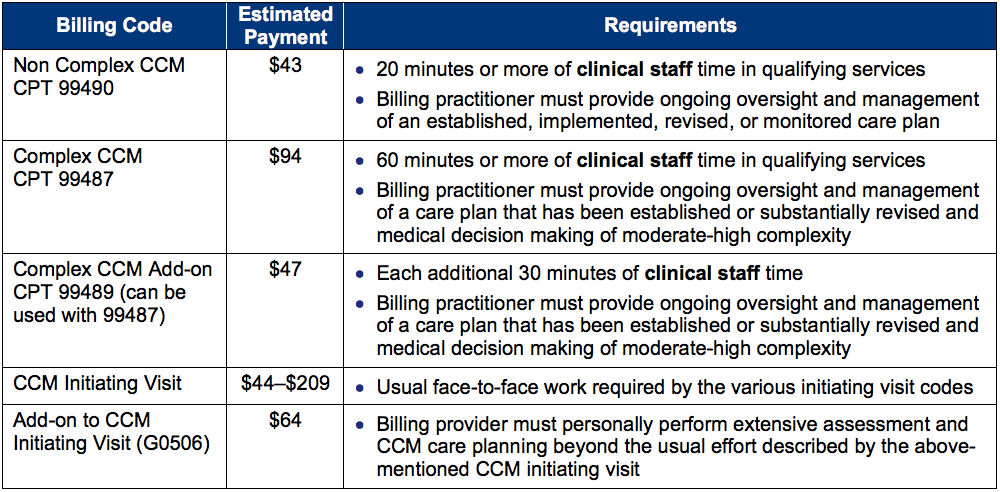
CCM codes are designed to help patients receive comprehensive management of their chronic diseases. The revised codes allow practices to be reimbursed for tasks they have previously not been compensated for but, have provided. The codes pay for time spent by providers and their clinical staff completing the very necessary components of this valuable care enhancement code. The CCM codes have time thresholds for billing; the table below will help you identify the various billing components.
Summary of 2017 CCM Coding Changes
Source: Medicare Learning Network, Department of Health and Human Services, Centers for Medicare and Medicaid Services ICN 909433, December 2016
CCM can be very cumbersome to a practice. Prior to implementing CCM within your practice, it is highly recommended that you identify the strongest patient advocate among your current staff or hire someone dedicated to CCM. The person must be a strong educator and someone that will work to empower the patients and their families.
Before beginning the actual CCM process, your practice should create scripting and protocols for the CCM coordinator. The CCM coordinator should be fully versed in the guidelines governing CCM billing. You will also want to ensure that all clinical staff and providers that will be documenting for CCM are aware of what counts towards the time and how it should be documented. Just as with evaluation and management documentation, CCM documentation should be bulletproof!
Luckily, there are options if you think CCM would benefit your ability to provide better care for your patients, but think you don’t have the time to document five minutes here and five minutes there. There are companies now completing the CCM clinical staff requirements off site from your practice. With appropriate remote access to electronic medical records, they take care of the work that would have been completed by your clinical staff and receive a portion of the revenue. This leaves the provider only responsible for implementing, revising, or monitoring the care plan and for providing oversight and management after the initial extensive assessment.
If you want to complete CCM on site, but don’t know where to begin with creating the scripting and protocols, those components can be purchased from various vendors. Then, implement them into your practice and begin billing.
Building CCM into your practice can be a bit daunting, but with the right tools in place it is well worth your time and effort from both patient care and financial aspects.

